If I Have the Shits Can My Baby Breastfeed
- Review
- Open Admission
- Published:
Breastfeeding and the risk for diarrhea morbidity and bloodshed
BMC Public Health volume 11, Article number:S15 (2011) Cite this article
Abstruse
Background
Lack of exclusive breastfeeding among infants 0-5 months of historic period and no breastfeeding amongst children six-23 months of age are associated with increased diarrhea morbidity and bloodshed in developing countries. We approximate the protective effects conferred past varying levels of breastfeeding exposure against diarrhea incidence, diarrhea prevalence, diarrhea mortality, all-cause bloodshed, and hospitalization for diarrhea affliction.
Methods
Nosotros systematically reviewed all literature published from 1980 to 2009 assessing levels of suboptimal breastfeeding equally a risk factor for selected diarrhea morbidity and mortality outcomes. We conducted random furnishings meta-analyses to generate pooled relative risks by outcome and age category.
Results
We plant a large body of prove for the protective effects of breastfeeding against diarrhea incidence, prevalence, hospitalizations, diarrhea mortality, and all-cause mortality. The results of random effects meta-analyses of 18 included studies indicated varying degrees of protection beyond levels of breastfeeding exposure with the greatest protection conferred past exclusive breastfeeding among infants 0-v months of historic period and by any breastfeeding amid infants and young children half dozen-23 months of age. Specifically, not breastfeeding resulted in an backlog risk of diarrhea mortality in comparison to exclusive breastfeeding amongst infants 0-5 months of age (RR: ten.52) and to any breastfeeding among children aged half dozen-23 months (RR: 2.18).
Conclusions
Our findings support the current WHO recommendation for exclusive breastfeeding during the first 6 months of life as a primal child survival intervention. Our findings too highlight the importance of breastfeeding to protect against diarrhea-specific morbidity and bloodshed throughout the commencement 2 years of life.
Background
The benefits of breastfeeding on infant and child morbidity and mortality are well documented, with observational studies dating back to the 1960s and 1970s [1–4]. Studies show that human milk glycans, which include oligosaccharides in their free and conjugated forms, are role of a natural immunological machinery that accounts for the way in which man milk protects breastfed infants against diarrheal disease [5]. In addition, breastfeeding reduces exposure to contaminated fluids and foods, and contributes to ensuring adequate diet and thus not-specific immunity. Despite prove supporting the positive and price-effective health impacts of exclusive breastfeeding on child survival [six] the exercise in resource-poor areas of the world is depression. In Africa, Asia, Latin America, and the Caribbean, only 47-57% of infants less than 2 months and 25-31% of infants 2-five months are exclusively breastfed, and the proportion of infants six-11 months of historic period receiving whatsoever breastmilk is even lower [7].
Given that diarrheal disease accounts for approximately 1.34 1000000 deaths among children ages 0-59 months and continues to act as the second leading cause of death in this historic period grouping [8], it is of import to quantify the preventive effect of breastfeeding practices on diarrhea-specific morbidity and mortality. Very few individual studies have been designed or powered to detect the effects of breastfeeding practices on diarrhea-specific morbidity and mortality for children 0-23 months of age in resource-limited settings.
In 2001, a systematic review of 16 independent studies conducted by the WHO attempted to resolve the "weanling'south dilemma" in developing countries. The review, which assessed the furnishings of sectional breastfeeding for vi months versus 3-4 months with mixed breastfeeding thereafter, resulted in the recommendation to promote exclusive breastfeeding for the first 6 months of life [9]. More recently, the authors of the Lancet diet series published a random furnishings meta-analysis estimating the increased risk of diarrhea-specific morbidity and bloodshed among children younger than 2 years in relation to suboptimal breastfeeding practices [7]. While these estimates provide confirmation of the protective effect of breastfeeding, they were based on a limited data set, rather than a complete systematic review, and thus a more thorough and updated revision is warranted.
Edifice upon previous reviews, this systematic review and meta-analyses use carefully developed and standardized methods to focus on the effects of breastfeeding practices every bit they relate to diarrhea incidence, prevalence, mortality and hospitalization amidst children 0-23 months of age. Here we present a comprehensive systematic review and meta-analysis equally evidence to be utilized past the Lives Saved Tool (Listing) to model the result of breastfeeding practices on diarrhea-specific morbidity and mortality [10, 11]. The results of our analysis will serve as the basis for generating projections of child lives that could exist saved by increasing exclusive breastfeeding until 6 months of age and continued breastfeeding until 23 months of age.
Methods
We systematically reviewed all literature published from 1980 to 2009 to identify studies with data assessing levels of suboptimal breastfeeding as a adventure factor for diarrhea morbidity and mortality outcomes. We conducted our initial search on July 28, 2009 and two updated searches on Apr 8 and May v, 2010. All searches were completed in Pubmed, EMBASE, the Global Health Library Global Index and Regional Index, and the Cochrane central register for controlled trials using combinations of primal search terms: breastfeeding, breast milk, human milk, diarrhea, gastroenteritis, morbidity, mortality, infant and kid. To ensure the identification of all relevant literature, we also reviewed the references of included papers.
After initially screening for eligibility based on title and abstract, we thoroughly reviewed full publications for inclusion and exclusion criteria outlined a priori. Nosotros included randomized controlled trials (RCT), accomplice and observational studies that assessed suboptimal breastfeeding as a risk factor for at least one of the following outcomes: diarrhea incidence, diarrhea prevalence, diarrhea mortality, all-cause bloodshed, and diarrhea hospitalizations. Included studies were published in any linguistic communication from 1980 - 2009 and were conducted in developing countries with a target population of children 0-23 months of age. Nosotros excluded studies reporting diarrhea as a result of only 1 microbial cause, and those with unclear methodology or data in a form that could not be extracted for meta-analysis. We also excluded studies reporting exclusive breastfeeding for children across half dozen months of age and those declining to restrict the allocation of diarrhea outcomes to concurrent breastfeeding status. Additionally, we excluded morbidity studies with diarrhea retrieve beyond two weeks and mortality studies where the removal of deaths occurring within the first three to 7 days of life was not possible. For studies reporting outcomes stratified by HIV status, we but abstracted data on HIV-negative infants and children.
We abstracted information for each diarrhea outcome by breastfeeding exposure levels, which were classified co-ordinate to current WHO definitions (Table 1) [12, xiii]. To permit for the comparability of breastfeeding labels and definitions derived from studies published over multiple decades, during which time breastfeeding definitions and terms evolved, we assigned the exposure categories described by each study to a WHO category on the footing of the study's definition of that exposure category, non the authors' category characterization. The majority of discrepancies betwixt breastfeeding label and definition arose over the term 'sectional breastfeeding'. By current standards, 'exclusive breastfeeding' does not include the ingestion of annihilation other than breastmilk and prescribed vitamins and medications, and infants receiving not-nutritive liquids, such equally waters and teas, are classified as 'predominantly breastfed' [12]. This distinction was non formally recommended until 1988 when a meeting of the Interagency Group for Action on Breastfeeding first proposed the development of a fix of standardized breastfeeding definitions [14]. WHO officially integrated indicators differentiating between sectional and predominant breastfeeding in 1991 [12]. As such, for this review nosotros assumed the 'sectional breastfeeding' category was more accordingly labelled 'predominant breastfeeding' for studies published prior to 1991, unless the report specifically defined sectional breastfeeding according to the current definition.
For studies that grouped exclusively and predominantly breastfed infants into a 'fully breastfeeding' category, we employed a conservative arroyo in which fully breastfeeding exposure was treated as predominant. We excluded studies that combined exposures other than exclusive and predominant breastfeeding into ane breastfeeding category.
In this review nosotros did not seek to address the issue of early initiation of breastfeeding and prelacteal feeds. Thus, in assigning breastfeeding exposure, we did not differentiate between exclusive and predominant breastfeeding on the basis of receipt of prelacteal feeds during the showtime three days of life.
We extracted consequence measures and 95% confidence intervals from all included studies. In cases where relative adventure (RR) was not reported, nosotros generated RR and 95% conviction intervals using reported numerators and denominators.
We organized data into the following historic period strata: 0-28 days, 0-5 mos, 0-eleven mos, half dozen-11 mos, 12-23 mos, and 6-23 mos. We excluded studies with overarching age categories that could non exist collapsed; however, we included one diarrhea mortality written report grouping children 12-35 mos and applied its RR to the 12-23 mos analysis [15]. For infants aged 0-5 mos, we generated pooled event measures using exclusive, predominant, and partial breastfeeding as reference categories. For infants in the 0-xi mos category, we used partial and any breastfeeding as reference categories, and for all age categories extending from 6 or 12 months, we used any breastfeeding as the only reference category.
We conducted fixed effects meta-analyses to combine effect measures within a given report that had been reported separately for ages falling within the same category in our assay. To generate a combined result measure beyond studies, we ran a random effects meta-assay for each comparison. All meta-analyses were performed using the meta command in STATA 10.1 [xvi].
For each outcome of interest, we summarized the evidence past conducting an assessment of report quality and quantitative measures as per CHERG guidelines. Every bit per the CHERG grading system, the overall quality of show for each effect estimate receives a score on a four point continuum ('high', 'moderate', 'low', 'very low'), which is then used to either support or oppose its inclusion in the LiST model [11]. To farther evaluate the limitations of included studies, we created a scoring arrangement to appraise the caste to which studies had accounted for reverse causality and cocky-choice—two major forms of bias in assessing the association between breastfeeding and diarrhea morbidity and mortality. Opposite causation bias results when breastfeeding cessation is a directly consequence of diarrheal disease. Self-selection bias occurs when children are weaned because they became repeatedly sick or grew improperly while breastfed. Although, it has been reported that cocky-option or reverse causation tin can as well create bias in the contrary direction, with some mothers less likely to wean sick children [17]. These biases can be reduced by the post-obit iv methods: (i) exclusion of deaths or episodes occurring inside the offset 7 days of life; (2) exclusion of infants and young children from non-singleton and/or premature births and those with low birth weight, congenital abnormalities, and any other serious illnesses unrelated to the upshot of interest; (3) identification of breastfeeding exposure immediately prior to the onset of illness or mortality as opposed to that concurrent with outcome; (iv) cess of whether weaning was a direct consequence of illness or poor growth and exclusion of such infants or immature children if their inclusion significantly changes the effect measure [xviii]. Nether our scoring system, nosotros assigned a study 0.5-i point for failure to incorporate each of these iv methods, such that contrary causality was considered not likely, likely, and highly likely for studies with zero, 0.5-2 and two.5-4 points, respectively. The studies and the data extracted from each besides as details on scoring studies for reverse causality are available in additional file 1.
Results
The systematic literature review yielded 2375 unique publications, 71 of which contained data on suboptimal breastfeeding as a adventure factor for the identified outcomes of interest (Figure 1). A total of eighteen studies met all inclusion, exclusion, and analytical criteria and were included in the analysis [fifteen, 19–35]. Of these, 11 were prospective cohort, 4 were cross-sectional observational, and 3 were instance-control studies. The majority were conducted in Latin America (n=7) but also took identify in Africa (due north=4), Due south Asia (n=5), the Middle East (northward=2) and the Western Pacific (n=two) regions, with one written report reporting three different study locations. The numbers of studies included in each meta-analysis are listed in Tables 2, 3, 4.
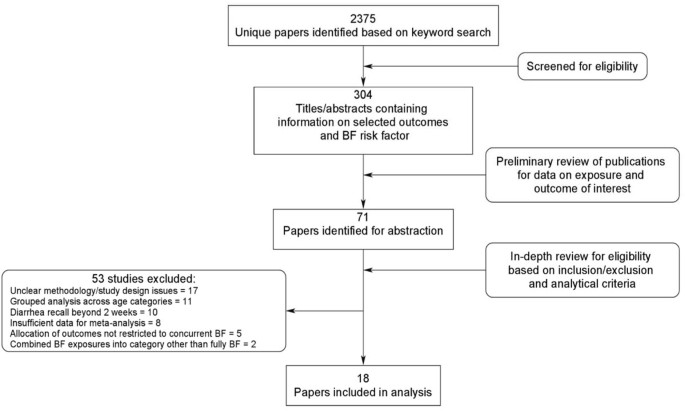
Synthesis of study identification in review process of the furnishings of suboptimal breastfeeding exposure on diarrhea incidence, prevalence, mortality, hospitalizations, and all-cause mortality
Diarrhea incidence
Amid infants 0-5 mos of age (Tabular array two), predominant (RR: one.26), partial (RR: 1.68) and non breastfeeding (RR: 2.65) resulted in an excess gamble of incident diarrhea in comparison to exclusive breastfeeding (Figures 2, 3). Similarly, the estimated relative risk of incident diarrhea was elevated when comparing not breastfed (RR: 1.32) to breastfed infants half-dozen-11 mos of historic period (Table iii; Effigy four). No studies reported diarrhea incidence comparing exclusive breastfeeding to suboptimal feeding among neonates.
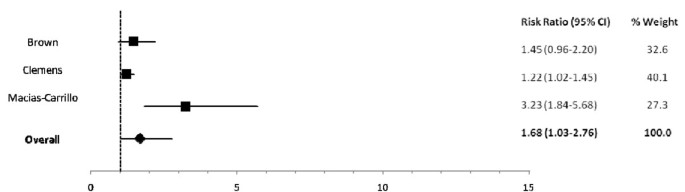
Woods plot for the effect of fractional breastfeeding as compared to exclusive breastfeeding on diarrhea incidence amongst infants 0-five months of age
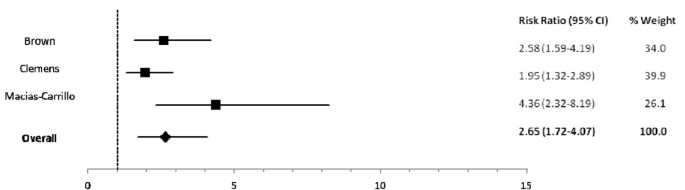
Wood plot for the consequence of non breastfeeding as compared to exclusive breastfeeding on diarrhea incidence among infants 0-5 months of age
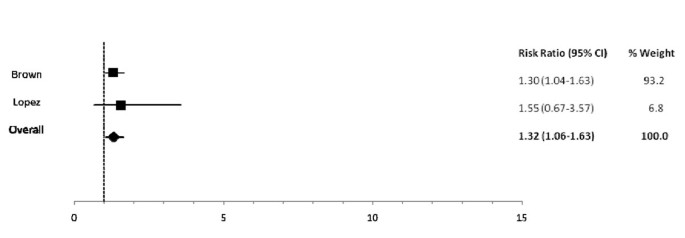
Forest plot for the upshot of non breastfeeding as compared to whatever breastfeeding on diarrhea incidence among infants half-dozen-11 months of age
Diarrhea prevalence
In comparison to exclusively breastfed infants 0-5 mos of historic period, the estimated relative risk of prevalent diarrhea was statistically significantly elevated in predominantly (RR: two.15), partially (RR: four.62), and not (RR: 4.90) breastfed infants (Table two). Among infants and immature children 6-23 mos of age (Table 3), not breastfeeding (RR: 2.07) resulted in an backlog risk of prevalent diarrhea as compared to breastfeeding. There were no studies comparing diarrhea prevalence amidst exclusively and suboptimally breastfed neonates (Table 4).
Diarrhea mortality
In comparison to exclusive breastfeeding, predominant (RR: 2.28), fractional (RR: 4.62) and non (RR: x.52) breastfeeding led to an elevated run a risk of diarrhea mortality amid infants 0-v mos of age (Table 2; Figures 5, 6, 7). Among infants 0-xi mos of age (Table two), the estimated risk of diarrhea mortality was higher in partially (RR: iv.19) and not (RR: eleven.73) breastfed infants equally compared to those predominantly breastfed. For infants and young children half dozen-23 mos of age (Tabular array 3), not breastfeeding (RR: 2.18) resulted in an excess risk of diarrhea mortality as compared to breastfeeding (Figure 8). In that location were no studies comparing the outcome of diarrhea mortality in exclusively versus suboptimally breastfed neonates (Table four).
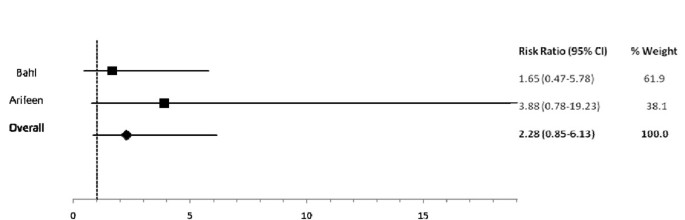
Forest plot for the effect of predominant breastfeeding as compared to exclusive breastfeeding on diarrhea mortality among infants 0-five months of age
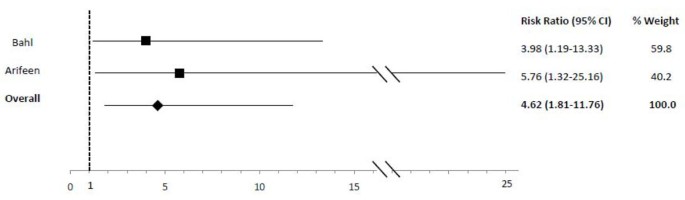
Woods plot for the effect of partial breastfeeding equally compared to exclusive breastfeeding on diarrhea mortality amongst infants 0-5 months of age
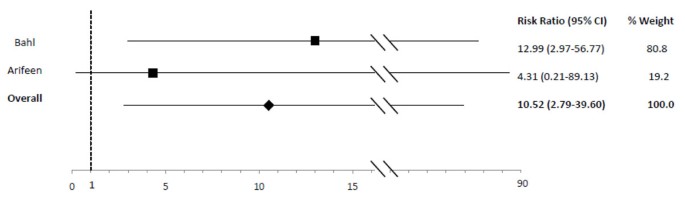
Forest plot for the effect of non breastfeeding as compared to exclusive breastfeeding on diarrhea bloodshed among infants 0-5 months of age
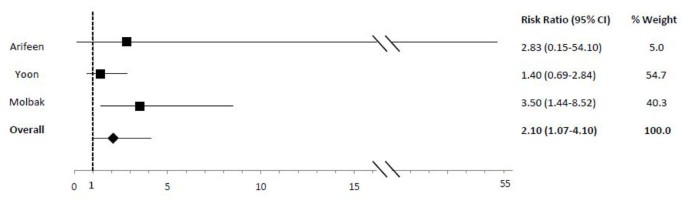
Forest plot for the effect of not breastfeeding equally compared to any breastfeeding on diarrhea mortality among infants 6-23 months of historic period
All-cause mortality
As compared to exclusively breastfed infants 0-5 mos of age (Table 2), the estimated relative risk of all-cause mortality was statistically significantly elevated among those predominantly (RR: 1.48), partially (RR: two.84) and not (RR: xiv.twoscore) breastfed. The estimated relative adventure of all-cause mortality was higher when comparison not breastfed (RR: three.69) to breastfed infants and young children 6-23 mos of age (Table 3). Among neonates, predominant (RR: 1.41), fractional (RR: 2.96), and no (RR: ane.75) breastfeeding resulted in elevated adventure of mortality as compared to exclusive breastfeeding (Table 4).
Diarrhea hospitalizations
The estimated relative gamble of hospitalization for diarrhea illness was elevated amid predominantly (RR: 2.28), partially (RR: 4.43) and non (RR: 19.48) breastfed infants 0-5 mos of historic period equally compared to those exclusively breastfed (Table 2). Amidst infants six-11 mos of historic period (Table 3), not breastfeeding continued to result in a higher risk of hospitalization for diarrhea when compared to whatever breastfeeding (RR: 6.05). There were no studies reporting diarrhea hospitalizations equally an upshot for neonates (Tabular array 4).
Quality assessment and effect size estimates for List
In tabular array five, we report the quality assessment of studies by outcome. Using the CHERG grading arrangement for report design and written report quality [11], outcome-specific quality was moderate for all outcomes of interest. Although reverse causation bias was probable or highly likely in the majority of studies, issue-specific findings were largely consequent with all simply ii studies confirming the highly protective effect of exclusive breastfeeding and whatsoever breastfeeding among infants 0-5 mos of age and young children 6-23 mos of age, respectively.
Applying the CHERG standard rules, potent prove exists for the reduction of diarrhea incidence and diarrhea mortality by exclusive breastfeeding among infants 0-5 mos of age and past whatsoever breastfeeding among children 6-23 mos of age. In tabular array 6, we present the final effect size estimates to be entered into LiST.
Discussion
We found a sizable body of evidence for the protective effects of breastfeeding against diarrhea incidence, prevalence, hospitalizations, diarrhea mortality, and all-cause bloodshed. The results of random effects meta-analyses of eighteen included studies indicated varying degrees of protection across levels of breastfeeding exposure [15, xix–35] .
For all outcomes among infants 0-5 mos of historic period, the protection conferred by exclusive breastfeeding was incrementally greater than that granted past predominant and fractional breastfeeding (Table 2). Our results also confirmed a protective effect of whatsoever breastfeeding against all outcomes among infants six-23 mos of age. The information for neonates alone are limited in that comparisons to sectional breastfeeding, the WHO recommendation for this age group, were not reported for four out of the five identified outcomes of involvement. Overall, our estimated effect sizes were large, thus suggesting a protective effect of breastfeeding among neonates.
The protection conferred by breastfeeding appears to operate via two pathways, decreasing diarrhea incidence as well every bit duration. The effect sizes appear to be larger for the reduction of diarrhea prevalence every bit compared to incidence suggesting that the predominate mechanism past which breastfeeding reduces diarrhea bloodshed is through the reduction of prolonged episodes.
In comparison to the Lancet nutrition serial [7], we study issue estimates for two additional outcomes—diarrhea prevalence and diarrhea hospitalizations, also every bit additional estimates for neonates separate from the 0-5 months historic period category. We also conducted meta-analyses comparing reference groups other than exclusive breastfeeding for infants 0-5 months of historic period. The results of our systematic review closely mirrored the final data ready included in the Lancet diet series and thus study nearly identical effect estimates for the meta-analyses of all-cause bloodshed for 0-v mos and 6-23 mos; diarrhea mortality for 0-5 mos; and diarrhea incidence for predominantly compared to exclusively breastfed infants 0-5 mos of age. We excluded two previously included studies on the basis of diarrhea recall across 2 weeks [36, 37], and we included iv additional studies not cited by the Lancet nutrition series [15, 23, 28, 35]. This resulted in lower consequence estimates than those previously reported for the take chances of diarrhea bloodshed and incidence in not breastfed children 6-23 mos of historic period and for the risk of incident diarrhea in partially and not breastfed infants 0-5 mos of age. Although we included i of the 3 studies included by the Lancet nutrition serial in the interpretation of the risk of diarrhea incidence among children 6-23 mos [22], we further stratified our results in this age category and thus study this RR under six-eleven rather than 6-23 mos. Overall, our results confirm and expand upon the protective furnishings of breastfeeding as previously reported by the Lancet nutrition serial.
Although the majority of studies included in this review did non methodologically account for the possibility of opposite causation, it is highly unlikely that this potential bias was responsible for the large issue sizes and consistent findings observed beyond all historic period categories and outcomes. This assertion is evidenced by the comparability of findings before and after adjusting for reverse causality inside included studies [4, 18, 20, 24]. Repeat analyses excluding all deaths occurring within 7 days of a feeding assessment did non statistically significantly alter the event measures observed by Bahl et al [twenty]. Similarly, the adjusted odds ratio (2.xl; 95% CI: 1.69-three.40) reported by Edmond et al. was very similar to the ORs observed afterwards excluding infants dying inside the beginning week of life (OR: ii.36; 95% CI: one.44-iii.87) or those at high take a chance of death due to premature birth, congenital anomaly, or ill health at the fourth dimension of interview (OR: 2.44; 95% CI: 1.60-three.74) [24]. Despite observing substantially higher relative risks before methodologically accounting for reverse causality, the stiff protective result of breastfeeding noted by Victora et al. persisted following this adjustment [4, eighteen].
While the current analysis was limited past a lack of geographic variety by outcome, the geographic diversity of the overall analysis was actually quite wide with studies taking place in eleven unique countries and in all WHO regions except Europe.
Additionally, the electric current assay was express in that effect measures from studies publishing raw data or estimates in a form insufficient for meta-assay were computed without correcting for potential confounders to breastfeeding exposure, such as socioeconomic status. All the same, we do not expect this to constitute a major limitation since similar methodology has been used in previous studies and since the direction and magnitude of effect sizes were consistent when comparing studies with and without controls for misreckoning. Furthermore, lack of aligning for misreckoning may have really led to an underestimation of the protective effect of breastfeeding, since poverty is associated with longer breastfeeding duration in many of the developing country populations included in this analysis [38].
The quality assessment resulted in a score of moderate outcome-specific quality (Tabular array v). Co-ordinate to CHERG standards, the overall score of moderate quality across all outcomes of this analysis indicates that these information represent the best available estimate of the protective issue of breastfeeding confronting diarrhea-specific morbidity and mortality and can therefore be included in the LiST model with confidence [eleven].
WHO and UNICEF currently recommend exclusive breastfeeding for the first vi mos of life with continued feeding through the beginning year among HIV positive mothers, provided that they or their infants receive ARV drugs during the breastfeeding catamenia.[39] In this review nosotros did not attempt to quantify the relative risks of alternative baby feeding practices in HIV positive populations. Though there are numerous studies suggesting that exclusive breastfeeding during the offset 6 mos and connected breastfeeding for the 2d 6 mos decrease mortality among infants born to HIV positive mothers [xl, 41], farther research is warranted every bit to whether the result sizes reported here are relevant among HIV positive mothers and infants.
Conclusions
In conclusion, our data confirm and highlight the importance of breastfeeding for the prevention of diarrhea morbidity and mortality. This review also provides updated risk estimates across age categories. Among infants 0-5 mos of age, these findings back up the recommendation for exclusive breastfeeding during the showtime half-dozen months of life as a cardinal kid survival intervention. Furthermore, results among infants and children beyond the first 6 mos of age reveal the importance of connected breastfeeding equally a critical intervention to protect against diarrhea-specific morbidity and mortality throughout the first two years of life. Though nosotros have confidence in the strength of the testify presented hither, continued research will be needed to update the effect size estimates every bit diarrhea and all cause mortality rates proceed to pass up in many developing countries.
This review does non evaluate the effect of breastfeeding promotion strategies or the operational challenges of inspiring mothers to commit to exclusive breastfeeding for the first vi months and to continued breastfeeding for the following 18 months. Operations research is needed to identify methods for maximizing the effectiveness of breastfeeding promotion programs and policies on behaviour change among mothers.
References
-
Gordon JE, Chitkara ID, Wyon JB: Weanling diarrhea. Am J Med Sci. 1963, 245: 345-377.
-
Waterlow JC, Thomson AM: Observations on the adequacy of breast-feeding. Lancet. 1979, 2: 238-242. ten.1016/S0140-6736(79)90248-4.
-
Bauchner H, Leventhal JM, Shapiro ED: Studies of breast-feeding and infections. How good is the testify?. JAMA. 1986, 256: 887-892. 10.1001/jama.256.vii.887.
-
Victora CG, Smith PG, Vaughan JP, Nobre LC, Lombardi C, Teixeira AM, Fuchs SC, Moreira LB, Gigante LP, Barros FC: Babe feeding and deaths due to diarrhea. A case-control written report. Am J Epidemiol. 1989, 129: 1032-1041.
-
Morrow AL, Ruiz-Palacios GM, Jiang 10, Newburg DS: Human-milk glycans that inhibit pathogen bounden protect breast-feeding infants against infectious diarrhea. J Nutr. 2005, 135: 1304-1307.
-
Riordan JM: The price of non breastfeeding: a commentary. J Hum Lact. 1997, 13: 93-97. ten.1177/089033449701300202.
-
Blackness RE, Allen LH, Bhutta ZA, Caulfield LE, de Onis Grand, Ezzati Thou, Mathers C, Rivera J: Maternal and child undernutrition: global and regional exposures and health consequences. Lancet. 2008, 371: 243-260. 10.1016/S0140-6736(07)61690-0.
-
Black RE, Cousens Southward, Johnson HL, Lawn JE, Rudan I, Bassani DG, Jha P, Campbell H, Walker CF, Cibulskis R, et al: Global, regional, and national causes of child mortality in 2008: a systematic analysis. Lancet. 2010
-
Kramer MS, Kakuma R: The Optimal duration of exclusive breastfeeding: A systematic review. Cochrane Database Syst Rev. 2002, CD003517-
-
Victora CG: LiST: using epidemiology to guide child survival policymaking and programming. Int J Epidemiol. 2010, 39: 650-652. x.1093/ije/dyq097.
-
Walker N, Fischer-Walker C, Bryce J, Bahl R, Cousens S: Standards for CHERG reviews of intervention effects on kid survival. Int J Epidemiol. 2010, 39 (Suppl 1): i21-31. x.1093/ije/dyq036.
-
Indicators for assessing breastfeeding practices. World Wellness System. 1991, WHO/CDD/SER, 91: fourteen-
-
Indicators for assessing baby and young child feeding practices. World Health Organization. 2007, WHO/CDD/SER, 07: fourteen-
-
Labbok K, Krasovec M: Toward consistency in breastfeeding definitions. Stud Fam Plann. 1990, 21: 226-230. 10.2307/1966617.
-
Molbak K, Gottschau A, Aaby P, Hojlyng N, Ingholt 50, da Silva AP: Prolonged chest feeding, diarrhoeal disease, and survival of children in Guinea-Bissau. BMJ. 1994, 308: 1403-1406. 10.1136/bmj.308.6941.1403.
-
Stata Corp. Statistical Software: Release x.1. 2008, College Station, TX: Stata Corporation
-
Marquis GS, Diaz J, Bartolini R, Creed de Kanashiro H, Rasmussen KM: Recognizing the reversible nature of child-feeding decisions: breastfeeding, weaning, and relactation patterns in a shanty town community of Lima, Peru. Soc Sci Med. 1998, 47: 645-656. x.1016/S0277-9536(98)00130-0.
-
Victora CG: Example-control studies of the influence of breastfeeding on child morbidity and mortality: methodological bug. Breastfeeding nutrition, infection and infant growth in developed and emerging countries. Edited by: Atkinson SA, Hanson LA, Chandra RK, .St Johns. 1990, Newfoundland: ARTS Biomedical Publishers and Distributors, 405-418.
-
Arifeen S, Blackness RE, Antelman G, Baqui A, Caulfield Fifty, Becker South: Exclusive breastfeeding reduces acute respiratory infection and diarrhea deaths among infants in Dhaka slums. Pediatrics. 2001, 108: E67-10.1542/peds.108.4.e67.
-
Bahl R, Frost C, Kirkwood BR, Edmond K, Martines J, Bhandari Northward, Arthur P: Infant feeding patterns and risks of expiry and hospitalization in the first one-half of infancy: multicentre cohort study. Bull Globe Health Organ. 2005, 83: 418-426.
-
Briend A, Wojtyniak B, Rowland MG: Breast feeding, nutritional country, and kid survival in rural Bangladesh. Br Med J(Clin Res Ed). 1988, 296: 879-882. 10.1136/bmj.296.6626.879.
-
Chocolate-brown KH, Black RE, Lopez de Romana M, Creed de Kanashiro H: Infant-feeding practices and their relationship with diarrheal and other diseases in Huascar (Lima), Republic of peru. Pediatrics. 1989, 83: 31-40.
-
Clemens J, Elyazeed RA, Rao Chiliad, Savarino Due south, Morsy BZ, Kim Y, Wierzba T, Naficy A, Lee YJ: Early on initiation of breastfeeding and the risk of infant diarrhea in rural Arab republic of egypt. Pediatrics. 1999, 104: e3-10.1542/peds.104.1.e3.
-
Edmond KM, Zandoh C, Quigley MA, Amenga-Etego S, Owusu-Agyei South, Kirkwood BR: Delayed breastfeeding initiation increases risk of neonatal bloodshed. Pediatrics. 2006, 117: e380-386. 10.1542/peds.2005-1496.
-
Garrido F, Borges Grand, Cardenas V, Bobadilla JL, Ibarra J, Ruiz-Matus C: Postneonatal mortality caused by diarrhea: a example-command report. Salud Publica Mex. 1990, 32: 261-268.
-
Ketsela T, Asfaw M, Kebede D: Patterns of breast feeding in western Federal democratic republic of ethiopia and their relationship to acute diarrhoea in infants. J Trop Pediatr. 1990, 36: 180-183.
-
Lopez-Alarcon Chiliad, Villalpando S, Fajardo A: Breast-feeding lowers the frequency and elapsing of astute respiratory infection and diarrhea in infants under half dozen months of age. J Nutr. 1997, 127: 436-443.
-
Macias-Carrillo C, Franco-Marina F, Long-Dunlap K, Hernandez-Gaytan SI, Martinez-Lopez Y, Lopez-Cervantes M: Chest feeding and the incidence of acute diarrhea during the first three months of life. Salud Publica Mex. 2005, 47: 49-57.
-
Mahmood DA, Feachem RG, Huttly SR: Infant feeding and adventure of severe diarrhoea in Basrah urban center, Iraq: a case-control written report. Balderdash World Health Organ. 1989, 67: 701-706.
-
Mihrshahi South, Oddy WH, Peat JK, Kabir I: Association between infant feeding patterns and diarrhoeal and respiratory illness: a accomplice study in Chittagong, Bangladesh. Int Breastfeed J. 2008, 3: 28-
-
Mulder-Sibanda M, Sibanda-Mulder FS: Prolonged breastfeeding in People's republic of bangladesh: indicators of inadequate feeding practices or mothers' response to children's poor health?. Public Health. 1999, 113: 65-68. x.1016/S0033-3506(99)00120-one.
-
Popkin BM, Adair Fifty, Akin JS, Blackness R, Briscoe J, Flieger W: Chest-feeding and diarrheal morbidity. Pediatrics. 1990, 86: 874-882.
-
Victora CG, Smith PG, Vaughan JP, Nobre LC, Lombardi C, Teixeira AM, Fuchs SM, Moreira LB, Gigante LP, Barros FC: Evidence for protection by chest-feeding against babe deaths from infectious diseases in Brazil. Lancet. 1987, 2: 319-322. 10.1016/S0140-6736(87)90902-0.
-
Vieira GO, Silva LR, de OVT: Child feeding and diarrhea morbidity. J Pediatr (Rio J). 2003, 79: 449-454.
-
Yoon PW, Black RE, Moulton LH, Becker S: Effect of non breastfeeding on the risk of diarrheal and respiratory bloodshed in children under 2 years of age in Metro Cebu, The Philippines. Am J Epidemiol. 1996, 143: 1142-1148.
-
Kumar Five, Kumar L, Diwedi P: Morbidity related to feeding pattern in privileged urban and nether privileged rural infants. Indian Pediatr. 1981, 18: 743-749.
-
al-Ali FM, Hossain MM, Pugh RN: The associations between feeding modes and diarrhoea amidst urban children in a newly developed state. Public Wellness. 1997, 111: 239-243. 10.1016/S0033-3506(97)00041-3.
-
Contemporary patterns of chest-feeding: report on the WHO Collaborative Study on Breast-feeding. Volume Contemporary patterns of chest-feeding: report on the WHO Collaborative Study on Breast-feeding. 1981, Metropolis:Geneva Switzerland: World Health Organization, 211: 24-
-
Guidelines on HIV and infant feeding: principles and recommendations for baby feeding in the context of HIV and a summary of evidence. Book Guidelines on HIV and infant feeding: principles and recommendations for infant feeding in the context of HIV and a summary of prove. 2010, City: Geneva Switzerland: World Wellness Organization
-
Homsy J, Moore D, Barasa A, Were Due west, Likicho C, Waiswa B, Downing R, Malamba S, Tappero J, Mermin J: Breastfeeding, female parent-to-child HIV transmission, and mortality among infants born to HIV-Infected women on highly agile antiretroviral therapy in rural Republic of uganda. J Acquir Immune Defic Syndr. 2010, 53: 28-35. 10.1097/QAI.0b013e3181bdf65a.
-
Coovadia HM, Rollins NC, Bland RM, Piffling K, Coutsoudis A, Bennish ML, Newell ML: Mother-to-child transmission of HIV-ane infection during exclusive breastfeeding in the start 6 months of life: an intervention cohort study. Lancet. 2007, 369: 1107-1116. 10.1016/S0140-6736(07)60283-9.
Acknowledgements
The study was supported past a grant from the Pecker and Melinda Gates Foundation to the US Fund for UNICEF for the ongoing piece of work of the Child Wellness Epidemiology Reference Group.
This article has been published as part of BMC Public Health Volume 11 Supplement three, 2011: Technical inputs, enhancements and applications of the Lives Saved Tool (Listing). The full contents of the supplement are available online at http://www.biomedcentral.com/1471-2458/11?issue=S3.
Author information
Affiliations
Corresponding author
Additional data
Competing interests
The authors have no competing interests.
Authors' contributions
LML conducted the systematic review, analysis and led the initial manuscript grooming. CLFW assisted with the analysis and the manuscript preparation. AN contributed to the systematic review, data brainchild, and manuscript preparation. CV and REB provided technical leadership and assisted with the interpretation of the assay and the final manuscript preparation.
Electronic supplementary cloth
12889_2011_2951_MOESM1_ESM.xlsx
Additional file 1: Breastfeeding and Diarrhea The additional file i is an excel spreadsheet named Final_Web_Appendix. This file contains 2 sheets. The 'Data Brainchild' canvass includes all data abstracted from studies, as well every bit notes on methodology and limitations. The 'Reverse Causality' sheet includes the assessment sheet used to systematically score studies on reverse causation bias. (XLSX 61 KB)
Rights and permissions
Open Access This article is published under license to BioMed Cardinal Ltd. This is an Open Access article is distributed under the terms of the Creative Commons Attribution License ( https://creativecommons.org/licenses/by/2.0 ), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Reprints and Permissions
About this article
Cite this article
Lamberti, L.M., Fischer Walker, C.L., Noiman, A. et al. Breastfeeding and the run a risk for diarrhea morbidity and mortality. BMC Public Wellness 11, S15 (2011). https://doi.org/ten.1186/1471-2458-11-S3-S15
-
Published:
-
DOI : https://doi.org/10.1186/1471-2458-eleven-S3-S15
Keywords
- Diarrhea
- Exclusive Breastfeed
- Diarrhea Prevalence
- Diarrhea Incidence
- Partial Breastfeed
Source: https://bmcpublichealth.biomedcentral.com/articles/10.1186/1471-2458-11-S3-S15
Post a Comment for "If I Have the Shits Can My Baby Breastfeed"